DIPG DMG National Brain Tumor Board
Offering treating providers of Diffuse Midline Gliomas, including Diffuse Intrinsic Pontine Gliomas, patient centered advice on innovative treatment options and clinical trials.
To be evaluated for the DIPG DMG National Brain Tumor Board, please complete the following information. Our coordinator will contact the patient provider within three business days of submittal.
What is DIPG and DMG?
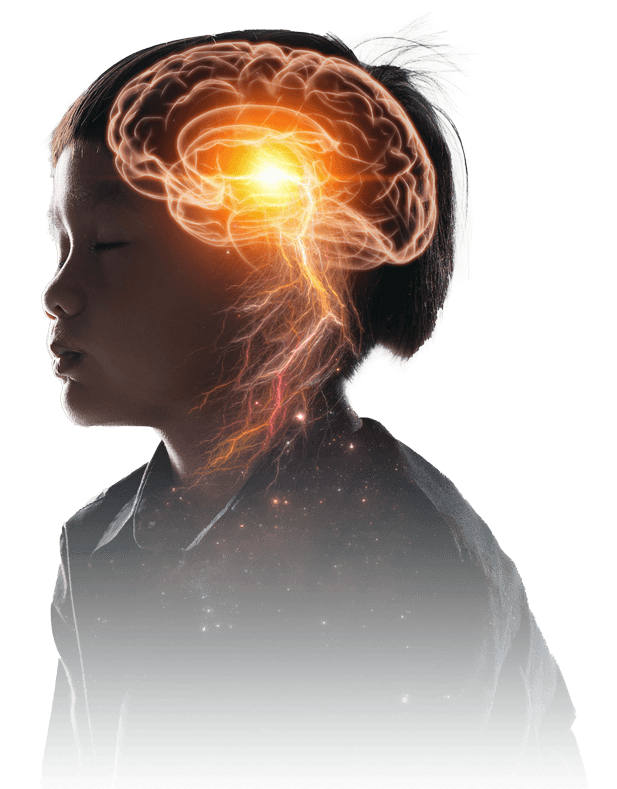
Diffuse Midline Gliomas (DMG), including Diffuse Intrinsic Pontine Gliomas (DIPG) are World Health Organization Grade IV pediatric diffuse high-grade gliomas. These are highly aggressive and difficult to treat malignant gliomas which progress rapidly. DMG is found in the lowest, stem-like part of the brain called the brainstem. The formation of DMG may be linked to brain development when cerebral tissue development is very active. Both astrocytic and oligodendroglia morphology has been recognized in DMG cells. Often DMG is centered in the pons (DIPG) which is considered the control center of the brain. For many years this cancer type, when centered in the pons, was known as DIPG, and among parent support groups and foundations is still called DIPG. DMG is more commonly used among providers and may include areas impacted in the thalamus, midbrain, spinal cord and extending into the cerebellum.
For over sixty years there has not been a change in the standard of care for DMG. During this time leading DMG DIPG clinicians have adjusted practices, offered clinical trials and have attempted to improve progression free survival, outside survival and the overall quality of life of patients. By gathering the experience of these clinicians, harnessing the power of the patient’s data in real time when possible and working together with committed researchers and providers, we believe a better future for those with DIPG/DMG is within reach. We believe in the power of working together with providers across the country to discuss ideas and forge solutions
When DMG Attacks the Brainstem
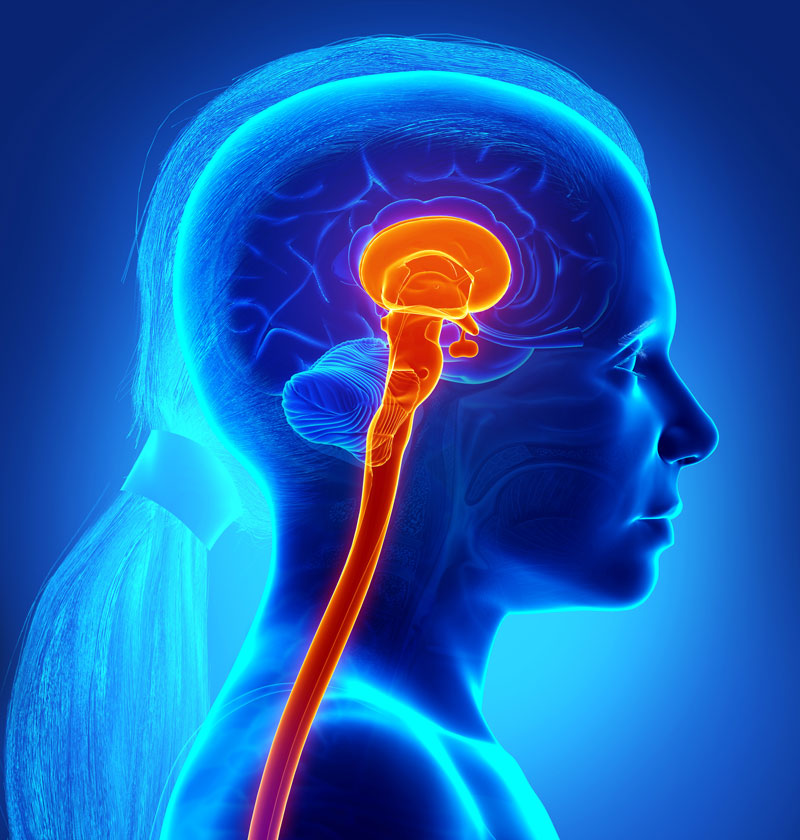
Many of the body’s most vital functions such a blood pressure, breathing and heart rate, as well as speech, swallow, control of eye movement, hearing, and control of the limbs are regulated within the pons. Normally, glial cells surround, support, and protect other cells. However, the small cancerous DMG cells infiltrate the gray and white matter creating a diffused web weaving through the brainstem where the cerebral function meets nerve impulse. The cells hijack the functions within the brainstem while causing inflammation to impair the functions of the pons, and in some cases the thalamus, spinal cord, and cerebellum.
DMG DIPG by the Numbers
DMG is considered terminal upon diagnosis with an estimated life expectancy of six to twelve months. It is found equally in boys and girls and generally is most common in children ages six to twelve years. However, children younger than the average range and individuals well into adulthood are also diagnosed with the same lethality. Brain cancer accounts for 26% of all childhood cancer the most deaths by disease in children. While there are four general groups of diffuse gliomas recognized in the 2021 WHO classification: 1) adult-type diffuse gliomas, 2) pediatric-type diffuse low-grade gliomas, 3) pediatric-type diffuse high-grade gliomas, and 4) circumscribed astrocytic gliomas, DMG and DIPG refer to the diffused high-grade gliomas located in the brainstem midline. DMG accounts for approximately 10% of cancerous brain tumors. Around 80% of DMG cases have a H3K27 alteration. The WHO recognizes this classification as “pediatric diffused high-grade glioma H3K27 altered-grade IV”. Other subtypes recognized by the WHO 2021 classifications include IDH1 wildtype, H3 wildtype and H3 G344 mutation.
How is DMG Diagnosed?
MRI and Clinical Presentation
DMG is commonly diagnosed through clinical presentation and MRI imaging of the brainstem. At some centers MS Spectroscopy (MRS) is used to measure the concentration of metabolites in the tumor tissue as well. Generally, in DIPG, more than half of the enlarged pons will typically show an increased signal on the T2 FLAIR MRI sequence. DIPG are expansile, infiltrative tumors which involve at least 50% of the pons. While small areas of necrosis can enhance, generally the tumor will not show contrast enhancement. A brain MRI with pons, thalamus, and cerebellum as well as a MRI of the spine is recommended to located any leptomeningeal tumor dissemination or spinal seeding.
What are Early Symptoms Leading to Diagnosis?
Most early symptoms are first observed less than four weeks prior to diagnosis. The early symptoms seem to correspond with the location of the cranial nerves impacted such as ataxia, dysmetria, dysarthria, or long tract signs such as hyperreflexia, positive Babinski sign, or weakness. The tumor disrupts the passing of information from the brain to the body and makes it difficult to control the movement of the body parts and limbs. It is also possible the patient will experience early in diagnosis obstructive hydrocephalus. The symptoms may develop quickly near the time of diagnosis from a change in facial expression or eye movement to changes in speech, chewing and swallow. Within days there could be weakness in the arm and legs, a change in gait, coordination, or balance.
Over time, DIPG DMG is most likely to take the walk, talk, speech, swallow, use of hands and arms, eyesight, and hearing of the person impacted. Usually, one side of the body and the opposite side of the head is affected. Over time the symptoms will progress until this cancerous tumor takes the last breath and stops the heart of the person with DIPG/DMG. Generally, DIPG DMG will leave the cognitive abilities of the patient entirely intact. The patient will always know exactly what is happening. However, working together with the DIPG DMG National Brain Tumor Board, committed researchers and clinicians, we believe we will soon see a better future for those with DIPG/DMG.
DMG or LGG in the Brainstem
Both DMG and low-grade gliomas (LGG) occur within the brainstem and can be very difficult to distinguish. LGGs are very slow growing, well circumscribed or exophytic in character which provide treatment and surgical options not available for DMG. LGG’s are 95 % survivable at year five. To distinguish DMG from LGG prior to radiation treatments, it is important to consider the use of a biopsy, other new diagnostics as well as the assistance of the DIPG DMG National Brain Tumor Board for a second opinion. The tumor board, made up of pediatric neuro oncologists, with consulting neuro pathologists, neuro radiologists and neurosurgeons treat many DMG each year. The tumor board can assist in confirming the DMG diagnosis and can provide options for treatment, which will likely to be very different for LGG patients.
How is DIPG DMG Diagnosed?
DMG is commonly diagnosed through clinical presentation and MRI imaging of the brainstem. At some centers MS Spectroscopy (MRS) is used to measure the concentration of metabolites in the tumor tissue as well. Generally, in DIPG, more than half of the enlarged pons will typically show an increased signal on the T2 FLAIR MRI sequence. DIPG are expansile, infiltrative tumors which involve at least 50% of the pons. While small areas of necrosis can enhance, generally the tumor will not show contrast enhancement. A brain MRI with pons, thalamus, and cerebellum as well as a MRI of the spine is recommended to locate any leptomeningeal tumor dissemination or spinal seeding.
Using a Biopsy to Confirm Diagnosis & Determine Underlying Mutations
Use of a Biopsy in Diagnosis
A stereotactic biopsy or liquid biopsy through a lumbar puncture tap are minimally invasive and can be safely performed by those institutions experienced in these procedures. In the past, stereotactic biopsy was not routinely performed in patients with classic radiographic findings of DMG as biopsies of the pons were thought too risky and without clinical benefit. Recent studies have shown that safe biopsies can be routinely offered to patients at time of presentation.
Advantages of Biopsy
The potential advantages of obtaining tumor tissue are (i) confirmation of diagnosis, which is especially helpful in cases with indeterminate radiographic findings; (ii) determination of molecular features to allow for administration of targeted therapy; and (iii) the advancement of clinical and basic research efforts. Many clinical trials now prescribe whether a patient must have a certain histone mutation to be eligible for the clinical trial. Because tissue from biopsy is scarce and multiple tissue biopsies should generally not be performed, the DIPG DMG National Brain Tumor Board recommends a tissue biopsy be undertaken by an institution very familiar with stereotactic biopsy of the pons.
The DIPG DMG National Brain Tumor Board has released this biopsy protocol intended to provide quick results with robust analysis using tissue sparingly. Potentially, both stereotactic and liquid biopsies may provide the patient better classification of the tumor for precision treatment, and ongoing insight as to how treatment is impacting the tumor.
What to Gather from a Biopsy
Suggested information to be collected from a tissue biopsy includes whole genome sequencing, exome sequencing, methylation status and other omics information. The DIPG DMG National Brain Tumor Board assists providers in using the results to help confirm diagnosis, classification, and recommend protocols and clinical trials for which the patient may be suited. The ability to obtain tumor tissue has led to the discovery that roughly 80% of DIPGs alter the gene that encode for histone 3 (H3K27M mutation), which in turn influences epigenetic regulation ultimately leading to oncogenesis.
As liquid biopsies advance, patients may continue to monitor changes in the tumor using liquid biopsies. Currently, some members of the tumor board are also exploring next generation sequencing to detect as much as possible about the tumor including mutations, fusions, methylome profiling, biomarker presence and other powerful tools to better understand the tumor’s molecular alterations.
How is DIPG DMG Treated?
Currently the standard of care, which is now more than thirty years old, is radiation following diagnosis.
Radiation
Treatment begins immediately following diagnosis. Radiation oncologist plans radiation treatment which may include the standard 54 gry of radiation given over 30 doses, or an abbreviated course of radiation of 29 gry. Photon radiation and Proton radiation have been found equally effective. Care should be given to know whether the clinical trial a patient may seek to enter following radiation will accept any protocol of radiation with less than 54 gry. If so, fractionated radiation or photon or proton radiation with radiation sensitizers, or delivery of clinical trial drugs during radiation are available to try instead of the standard of care radiation. In some cases the pons will appear smaller or the tumor less dense after radiation.
Steroids to Control Inflammation
In the Best Practice for Newly Diagnosed, steroids are also discussed. Traditionally, steroids, specifically dexamethasone, is given at diagnosis with the goal of stabilizing the neurological symptoms until biopsy or radiation begins. However, complications due to long term and escalating dose steroid use should be avoided whenever possible. The patient family should be given information to assist in understanding the benefits of pulse dosing steroids and weaning off steroids when tolerated. Steroids stabilize the blood brain barrier and can affect tissue penetration of systemic therapies. Additionally, dexamethasone is associated with worse overall survival.
Shunts, Ommayas and apparatus to control CSF buildup
On occasion, in about 10% of all DMG DIPG patients, hydrocephalus occurs requiring relief of the buildup of cerebral spinal fluid (CSF). This may be managed with medication or installation of an Ommaya catheter, Ventricular Assisted Devise, or ventricular shunt. Some clinical trials exclude patients following the installation of certain apparatus reducing hydrocephalus. Therefore, the DIPG DMG National Brain Tumor Board recommends using the tumor board to consult with providers on the placement of such apparatus, the timing with respect to clinical trials of interest for the patient and for alternatives to shunts and steroids.
Clinical Trials and Protocols
Beyond these protocols more common in DIPG DMG treatment, Phase I or Phase II clinical trials are offered to evaluate the safety (in Phase I trials) or the efficacy (in Phase II trials) of proposed treatments. Clinical trials are listed at clinicaltrials.gov and routinely updated as to the status of recruiting, actively enrolling, or enrollment completed. To date, there is no cure for DIPG DMG. There is not one clinical trial that is proving successful in a majority of patients entering the trial. Yet, a small percentage of patients are outliving the two years outside life expectancy, many following enrollments in one or another clinical trial. New DIPG research may provide the key to improved personalized treatment options. It may help discover why one trial is working better for one patient and another trial works better for another patient. The DIPG DMG National Brain Tumor Board will to review clinical trial and compassionate protocol options with providers in order to shed light on best practices, by consensus, and trial recommendations for patient care.
Using the DIPG DMG National Brain Tumor Board
The DIPG DMG National Brain Tumor Board recommends using insight from the MRI, clinical notes and the reports from biopsy or liquid biopsy to inform the treating provider as to those clinical trials a patient would not likely be eligible to enter.
The DIPG DMG National Brain Tumor Board will issue a written report to the provider discussing those clinical trials of DIPG DMG and any protocols which may prove to benefit the patient. The status of clinical trials is constantly changing. The DIPG DMG National Brain Tumor Board, through its coordinator, strives to update the tumor board on the satus of available trials. This allows the board to consider options available across the country which may be suited for the patient under review.
However, working together with committed researchers and providers, we believe a better future for those with DIPG/DMG is within reach.
To submit a patient for DIPG DMG National Brain Tumor Board review complete this intake form or if you are a provider email DMGNationalTumorBoard@ucsf.edu
![Ronsley_Rebecca 004[91] copy-Photoroom Ronsley_Rebecca 004[91] copy-Photoroom](https://dmgnationaltumorboard.org/wp-content/uploads/2025/03/Ronsley_Rebecca-00491-copy-Photoroom.png)
The DIPG DMG National Brain Tumor Board also consults with the following when needed to complete its review:
Gerald Grant, MD, Neurosurgeon, (Duke Health Systems)
Nalin Gupta, MD, Neurosurgeon, (UCSF)
Matthew Barkovich, MD, Neuroradiologist (UCSF)
Why should a provider observe the DIPG DMG National Brain Tumor Board?

To know options to present to the patient for clinical trials, the status of those trials from people close to the trials, and protocols of compassionate care or treatment to consider outside of trials -- Consider this your think tank of solutions to offer from those who see DIPG DMG most often on what the next best steps might be within 12 weeks of diagnosis or 4 weeks following first progression.

To help place the patient on the radar of clinical trials enrolling across the country; to allow the patient family the opportunity to decide whether trial, compassionate protocol treatment or no treatment beyond standard of care is right for them

To learn from the tumor board -- what do those pediatric neuro oncologist who see many cases each year look for when evaluating newly diagnosed patients. What is most helpful in reviewing the MRI, results from biopsy, if any, and clinical presentation?

To network with providers who are exploring trial opportunities, and information to be gained from open access patient registries. Learn with others on the cutting edge of DIPG DMG about your patients and other patients like yours.
Why should a provider attend the DIPG DMG National Brain Tumor Board?

To know options to present to the patient for clinical trials, the status of those trials from people close to the trials, and protocols of compassionate care or treatment to consider outside of trials -- Consider this your think tank of solutions to offer from those who see DIPG DMG most often on what the next best steps might be within 12 weeks of diagnosis or 4 weeks following first progression.

To help place the patient on the radar of clinical trials enrolling across the country; to allow the patient family the opportunity to decide whether trial, compassionate protocol treatment or no treatment beyond standard of care is right for them.

To learn from the tumor board -- what do pediatric neuro oncologists, several who see more DIPG DMG cases than most, look for when evaluating newly diagnosed patients. What is most helpful in reviewing the MRI, results from biopsy, if any, and clinical presentation.

To network with providers who are exploring trial opportunities, and information to be gained from open access patient registries. Learn with others on the cutting edge of DIPG DMG about your patients and other patients like yours.
The DIPG DMG National Brain Tumor Board is funded by DDRFA
DDRFA is powered by families and foundations who know first-hand the journey of DIPG and DMG. Together, the members fund the DIPG DMG National Brain Tumor Board, basic and translational research, access to clinical trials and the use, integration and collection of patient derived data. Through DDRFA, our members work as fast as possible to fund and drive change because we are well aware lives depend on it. The DIPG DMG National Brain Tumor Board is also funded in part by the Elliot Rose Fund.









































































